Ear infections
Middle ear infections are also called otitis media. They are very common, especially in children between 6 months and 3 years of age. They are usually not serious. Although not contagious, the viral illness that caused the infection can be. Most ear infections happen when a child has already had a cold for a few days.
What causes an ear infection?
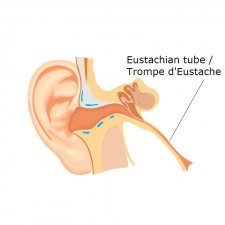
Viruses or bacteria (germs) cause middle ear infections. The eustachian tube connects the middle ear with the back of the throat. Germs travel from the back of the throat when the eustachian tube is swollen from a cold, causing infection in the middle ear.
Who is at higher risk for ear infections?
- Children less than 5 years old, because they have shorter eustachian tubes.
- Children who attend daycare, because they tend to have more colds.
- Children with allergies.
- Children who are exposed to cigarette smoke. Smoke causes inflammation of the eustachian tube, making ear infections more likely.
- Children who were not breastfed. Breast milk has antibodies that help fight infections.
- Babies who are being bottle-fed, especially if they swallow milk while lying too flat. Milk can enter the eustachian tube and cause inflammation, which increases the risk of an ear infection. Children should be held upright while drinking a bottle. When they are old enough to hold their own bottle well, they should be taught to drink from a regular cup (not a “sippy cup”) and no longer given a bottle.
- Children with cleft palates, as their eustachian tubes are often inflamed.
- Children of First Nations and Inuit descent, though it’s not clear why.
- Children with Down syndrome.
How do I know if my child has an ear infection?
Older children will usually complain of an earache. While younger children might not be able to say they have an earache, they may:
- have an unexplained fever,
- be fussy,
- have trouble sleeping,
- tug or pull at their ears, or
- have trouble hearing quiet sounds.
Some children with an ear infection may also have fluid draining from the ear.
How is an ear infection diagnosed?
Doctors diagnose ear infections by looking at the ear drum (tympanic membrane) with a special light called an otoscope. They look for fluid in the middle ear, at the colour and position of the ear drum, and monitor the pressure in the middle ear. Common viral infections can make the ear drum look red, but antibiotics are not needed.
How is an ear infection treated?
- If a child doesn’t have too much discomfort or a high fever, the doctor will likely wait 24 to 48 hours (1 to 2 days) to see if the ear infection gets better on its own. If the child does not improve or gets worse, contact the doctor again.
- You child’s doctor will prescribe antibiotics if:
- your child is moderately to severely ill with a high fever (more than 39◦C),
- your child has severe pain,
- the condition has not improved for 48 hours, or
- the ear canal has new fluid.
-
For an uncomplicated ear infection, children between 6 months and 2 years usually take an antibiotic for 10 days. Children over 2 years of age will take an antibiotic for 5 days.
-
The doctor might suggest acetaminophen or ibuprofen to reduce the child’s pain. Only give ibuprofen if your child is drinking reasonably well. Do not give ibuprofen to babies under 6 months old without first talking to your doctor.
-
Do not give over-the-counter medications (ones you can buy without a prescription) to babies and children under 6 years without first talking to your doctor. The only exceptions are medications used to treat fever, such as ibuprofen and acetaminophen.
Children usually feel better within 1 day of starting an antibiotic, but make sure to finish it. Your doctor might want to see your child again to be sure the infection has cleared up completely. Fluid can remain in the middle ear without inflammation for a few weeks.
When do children need tubes in their ears?
If your child has frequent ear infections, or if they have trouble hearing because of ongoing fluid in the middle ear, they may need a tube inserted through the eardrum and into the middle ear. The tube helps to keep air pressure normal on both sides of the ear drum and helps fluid drain from the middle ear.
Putting tubes in requires a brief operation by an ear, nose and throat surgeon. Children can usually go home the same day.
When should I call the doctor?
Call your doctor if you think your child has an ear infection AND:
- has other serious medical problems,
- seems ill,
- vomits over and over,
- is younger than 6 months old,
- is older than 6 months old and has had a fever for more than 48 hours,
- has redness and swelling behind the ear,
- is very sleepy,
- is very irritable,
- has a skin rash,
- isn’t hearing well or at all,
- remains in a lot of pain despite at least one dose of acetaminophen or ibuprofen, or
- still has an earache after 2 days of treatment with acetaminophen or ibuprofen.
How can I prevent my child from getting an ear infection?
- Wash your child’s hands and your own often to keep germs away.
- If possible, breastfeed your baby.
- Avoid bottle-feeding your baby when they are lying down. Never put your baby to bed with a bottle.
- Transition your baby from a bottle to a cup by 1 year of age.
- Don’t smoke, and keep your child away from any second-hand smoke. Exposure to smoke can increase the risk of ear infections.
- Ensure your child gets the pneumococcal vaccine (if they are at least 2 months of age, and have not already had this shot).
- Ensure your child gets a flu shot every year.
- If your child has had many ear infections, try reducing the use of pacifiers (soothers). Using a pacifier may increase the risk of repeated ear infections.
Additional resources
Reviewed by the following CPS committees
- Community Paediatrics Committee
Last updated: March 2022